Your Back
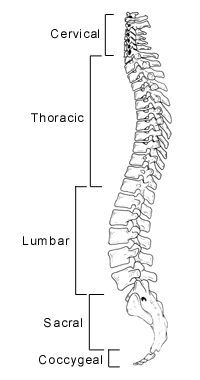
The spine is a multi-segmented column of approximately thirty-two bones (vertebrae). There are usually seven vertebrae that make up the cervical spine, twelve in the thoracic region and five in the lumbar region. The remainder form the sacrum and coccyx.
The spinal cord and nerve roots pass along the spinal canal inside a tube like membrane called the dural sac and the spinal cord and nerves are bathed by a watery fluid called cerebrospinal fluid or CSF. In an adult the spinal cord ends in the upper lumbar spine, usually at the level of the first lumbar vertebrae. Below this there are a number of nerves that pass down to the base of the spine in the spinal canal. These nerves pass out of the spinal canal between adjacent vertebrae and on to the arms, the trunk or the legs.
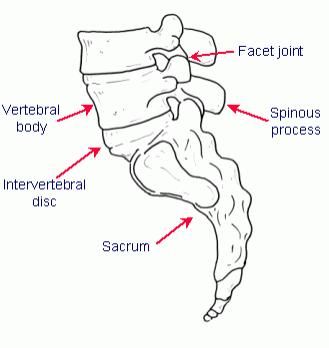
Each vertebra is linked to the vertebra above and below by an intervertebral “disc” at the front, and by two facet joints at the back.
The intervertebral disc consists of two parts, a tough outer part called the annulus, and a softer interior part called the nucleus pulposus. Discs act as “shock absorbers” and as we get older the consistency of the nucleus changes and deteriorates or degenerates.
The facet joints towards the back of the spine are similar in structure and function to other joints in the body and will also wear out or degenerate as we get older. Degeneration of both the discs and facet joints are part of the normal aging process. These changes are often widespread and can not be reversed.
Degeneration may be the source of back or neck pain, but in many cases this process does not result in significant ongoing pain.
Where pain does develop it is not uncommon for discomfort to be referred from the spine into the buttocks, thighs or even below the knee and into the calf or foot. Neck pain may also be referred into the shoulder or arms, and not uncommonly is also associated with headaches.
Back Pain
Back pain is extremely common with approximately eighty percent of the adult population experiencing a significant episode of low back pain at some time in their lives. In the majority of cases symptoms will resolve spontaneously, usually within six to twelve weeks. Studies show that back ache is more a problem of middle age than old age. This may be due to the fact that as we get older the demands on our body change and we tend to place less stress on our backs. It may also be that we learn to cope with back discomfort.
It is also true that as a joint wears out its range of movement is reduced. As it is often the movement of a degenerate joint that results in discomfort, as we get older and our joints get stiffer, pain tends to diminish. This increased stiffness does not usually cause a problem due to a reduction in the physical demands placed on our bodies with increasing age. Whatever the reason, by the time we reach our sixties the back pain that was disabling in our thirties or forties will usually settle to a nuisance ache.
It is important to remember that not all cases of back and leg pain are the same, even if the symptoms are very similar. Pain felt in the buttock, thigh or leg may be due to a variety of problems in or around the spine, and the diagnosis and treatment may vary widely according to the nature of the underlying problem. We will attempt to identify the origin of your pain through the examination undertaken and the investigations requested. This can take time.
“Mechanical back pain” is a term used to describe back, buttock and leg pain that results from degeneration of intervertebral discs and/or facet joints. Pain of this type is aggravated by loading, and relieved by unloading the spine. The intervertebral discs are loaded maximally when lifting and bending forward, but also when we sit. Facet joints tend to be loaded more when we bend backward, to the side or perform twisting movements. Mechanical back pain is usually episodic and you are likely to have good days and bad days, good weeks and bad weeks, good months and bad months. Symptoms may be aggravated by a particular incident or event, but may also develop gradually.
It is important to remember the degeneration evident on your X-rays, MRI or CT scan is the result of the wear and tear, and the stresses and strains or injuries your body has endured through your entire life. It is usually not possible to state with any certainty that a particular event caused these changes. It is in fact more common for specific events to result in nothing more than the acceleration or aggravation of this degeneration rather than its initiation
Wherever possible conservative or non-operative treatment is recommended. This may include limited bed rest for acute episodes of pain (ie. 2-3 days), medication including analgesics and/or anti-inflammatories and physical therapy.
The most important principle of non-operative or “conservative” treatment of back pain is to “unload” the spine by losing excessive weight and improving the muscular support of the spine through regular exercise. Exercises for specific muscle groups are important, but maintaining your general fitness through activities that do not jar the spine, such as walking, swimming, bike-riding and light gym programs is also very important.
If symptoms persist and are disabling, despite involvement in an adequate conservative program over an extended period, surgery may be considered.
The surgical treatment of this type of pain usually involves a spinal fusion. This should be considered as the last resort.
A spinal fusion is a major operation and is associated with some risk. It often takes between six and twelve months to recover fully from a spinal fusion and complete rehabilitation.
Surgery is therefore considered only if symptoms are disabling, interfere with both work and social activities and disturbs your sleep over an extended period of time.
A spinal fusion will therefore usually not be offered unless symptoms have been present for at least twelve months, and then only if the source of your pain has been identified. It is also our belief that surgery should only be contemplated if the potential benefits outweigh the inherent risks of the procedure, providing there is a reasonable chance that surgery will help your complaint.
