Sciatica is a term that describes pain extending from the buttock into the leg and which radiates below the knee.
Sciatica may result from a variety of conditions but is usually due to the compression or irritation of the lower lumbar nerve roots. Pain usually results from a disc protrusion or rupture, where disc material reduces the capacity of the spinal canal and results in the compression of a lumbar nerve root.
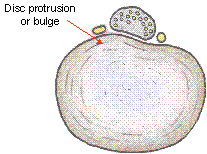

Disc bulges are a common finding on either a CT or MRI scan and may not be the cause of your leg or back pain.
In the majority of cases (90%), symptoms of sciatica will settle spontaneously within a six to twelve week period, and treatment is initially directed towards reducing discomfort so that you can remain active both at work and at home.
When leg pain due to a disc protrusion resolves there is only a 20 to 25% chance that symptoms will return in the future. Even if this should occur there is still a 90% chance that symptoms will again resolve within six to twelve weeks. As a result of this less than 10% of people with sciatica end up having surgery.
Treatment Options:
Wherever possible non-operative treatment is recommended. This may include a limited period of bed rest (usually no more than 2-3 days), physical therapy and medications such as analgesics and anti-inflammatories.
Where symptoms persist more invasive forms of treatment may be considered.
- Epidural Injection
- Partial discectomy
Irrespective of the outcome of interventional treatment for sciatica the offending disc is always degenerate and may subsequently be a cause of low back pain.
Epidural Injection:
An epidural steriod injection may be recommended as the initial treatment of sciatica. This may hasten the natural healing process and the resolution of pain.
Partial Discectomy:
A partial discectomy is performed under a general anaesthetic through a small incision, approximately 3cm long in the middle of your back. An x-ray is taken at the start of the procedure to mark where the incision should be made. The muscles are lifted off the bone and a ligament that lies between the vertebrae overlying the ruptured disc is removed. This is done in order to gain access to the spinal canal and enables removal of the ruptured disc and decompression of the affected nerve root.
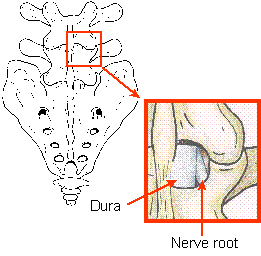
Only loose fragments of disc material are removed, as it is neither possible nor practical to remove the entire disc.
It is usual to begin mobilising on the day of surgery with the assistance of the nursing staff, and the hospital stay may vary from one to five days depending on your progress and home situation.
It is usual for buttock and leg pain (sciatica) to be relieved following surgery but there will be some post-operative back pain that usually settles as the muscles heal. The rate of recovery varies from patient to patient, but you will usually need to have between three and six weeks off work. Driving will be restricted until you can sit comfortably, brake and respond appropriately which will usually take approximately ten days.
Ninety percent of people obtain satisfactory relief of their sciatic symptoms with surgery of this type. There is however a 5% incident of a recurrent disc protrusion at the same level, and in a similar proportion of people disc degeneration will result in ongoing low back pain. The incidence of back pain is however similar whether you have surgery or not.
